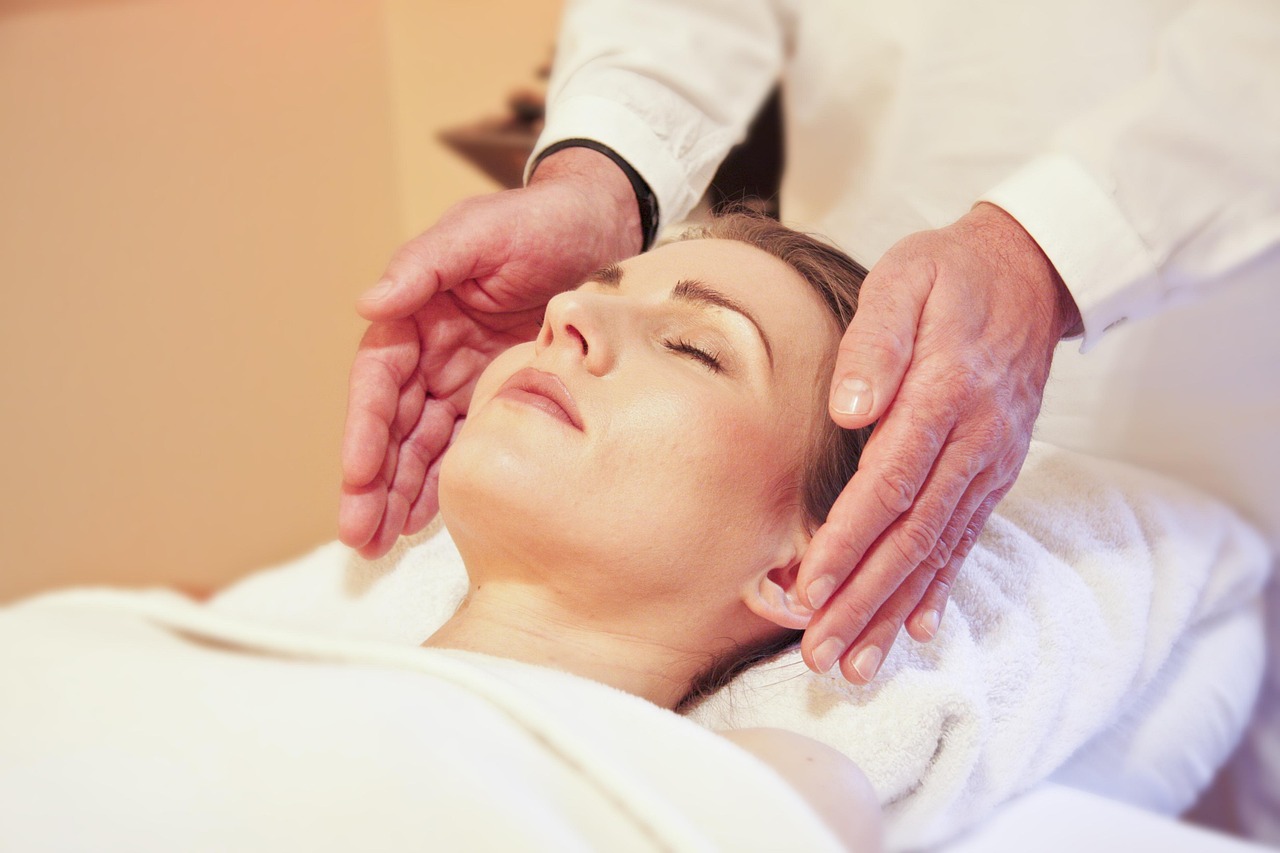
You can enter a focused, relaxed state that makes changing habits, easing pain, and reducing anxiety more effective than many people expect. Clinical hypnosis uses guided attention and suggestion, delivered by trained professionals, to help you access mental processes that support measurable therapeutic goals.
This article explains how clinical hypnosis works, what evidence supports its use, and which problems it helps most—so you can decide whether it fits your needs. Expect clear descriptions of techniques, practical examples of applications, and summaries of the research behind them to guide your next step.
Understanding Clinical Hypnosis
Clinic hypnosis helps you access focused attention and increased suggestibility to address specific symptoms, behaviors, or pain. It pairs guided relaxation and targeted suggestions with therapeutic goals, and is delivered by trained health professionals within a clinical framework.
Definition and Core Concepts
Clinical hypnosis is a therapeutic method that uses guided mental states—often called trance or focused attention—to encourage adaptive thoughts, emotions, and behaviors. You enter a state of concentrated attention and reduced peripheral awareness; this state increases responsiveness to carefully worded suggestions aimed at your specific goals.
Key elements you should know:
- Intentionality: the clinician sets clear therapeutic objectives with you.
- Suggestibility: you remain able to accept or reject suggestions; hypnosis does not remove your control.
- Safety and ethics: licensed clinicians combine hypnosis with evidence-based treatments and informed consent.
Clinical hypnosis is not sleep, mind control, or a stand-alone magic cure. It functions as a tool to augment psychotherapy, medical care, or behavioral interventions.
History and Development
Clinical hypnosis evolved from early practices in the 18th century to a modern, evidence-informed clinical tool. Practitioners trace origins to Mesmer’s animal magnetism and 19th-century demonstrations, but you see contemporary methods rooted in Milton Erickson’s brief, permissive techniques and later empirical research.
Over the past few decades, researchers moved from anecdote to randomized controlled trials and meta-analyses. Universities and hospitals now study hypnosis for pain, anxiety, and habit change. Training standards also shifted: reputable clinicians combine hypnosis training with formal credentials in psychology, medicine, or counseling.
You should expect clinical hypnosis to be integrated with other treatments rather than used in isolation, and standards of practice emphasize documented efficacy and patient safety.
How Clinical Hypnosis Works
Clinical hypnosis uses a structured process: induction, deepening, therapeutic suggestion, and reorientation. During induction you follow verbal cues to relax and narrow attention. Deepening techniques increase focus and physiological relaxation so therapeutic suggestions have greater impact.
Mechanisms supported by research include:
- Attention modulation: hypnosis concentrates conscious attention on targeted images or sensations.
- Expectancy and learning: your beliefs about treatment and repeated practice modify responses.
- Neurobiological changes: studies show altered activity in brain networks for attention, self-monitoring, and pain perception.
Typical applications involve symptom-specific scripts (pain reduction, smoking cessation, anxiety management) combined with cognitive or behavioral strategies. You remain aware and can stop the process at any time; clinicians document progress and adjust techniques to your responses.
Applications and Effectiveness of Clinical Hypnosis
Clinical hypnosis helps you manage physical symptoms, change unhelpful thoughts and behaviors, and reduce procedure-related distress. It applies across medical procedures, pain and symptom control, and psychological treatments using structured suggestion and focused attention.
Medical and Psychological Uses
You can use hypnosis as an adjunct or primary intervention in medical settings such as perioperative care, labor, and management of irritable bowel syndrome. In anesthesia-adjacent care, hypnotic communication and waking suggestions reduce anxiety and analgesic needs for some patients.
Hypnosis also helps with chronic pain, tension and migraine headaches, and some functional somatic syndromes by altering pain perception and coping responses.
On the psychological side, you can use hypnosis for anxiety disorders, phobias, PTSD, and smoking cessation. It assists exposure-based work and cognitive restructuring by increasing openness to targeted suggestions and accelerating skill acquisition.
Use is typically protocolized (e.g., hypnotic relaxation, Ericksonian approaches) and integrated with CBT or medical care.
Therapeutic Techniques
You will commonly encounter induction followed by deepening, targeted suggestion, and post-hypnotic cues. Inductions focus attention and reduce peripheral distraction; deepening stabilizes the trance for therapeutic work. Suggestions target symptom interpretation, habit change, or behavioral rehearsal.
Techniques vary: traditional direct suggestion aims at specific symptom relief, while Ericksonian and permissive methods use metaphor and indirect language to engage unconscious processes.
You may also see combined approaches such as guided imagery for pain, hypnotic relaxation for stress reduction, and suggestion-based behavior rehearsal for habit change. Session frequency ranges from a single preoperative intervention to multiple weekly sessions for chronic conditions.
Clinicians tailor scripts and homework to patient readiness and the clinical target.
Evidence and Research on Outcomes
Randomized controlled trials and meta-analyses support hypnosis for several specific outcomes. Stronger evidence exists for procedural anxiety reduction, irritable bowel syndrome symptom improvement, and certain pain conditions, where effect sizes are clinically meaningful.
Research quality has improved with RCTs, standardized protocols, and outcome measures, though heterogeneity in methods persists.
You should note limitations: not all conditions show consistent benefits, and placebo or expectancy effects can contribute. Predictors of better response include high hypnotizability, clear treatment targeting, and integration with concurrent therapies.
Ongoing meta-analyses and mechanistic studies continue to refine which techniques work best for which patients.